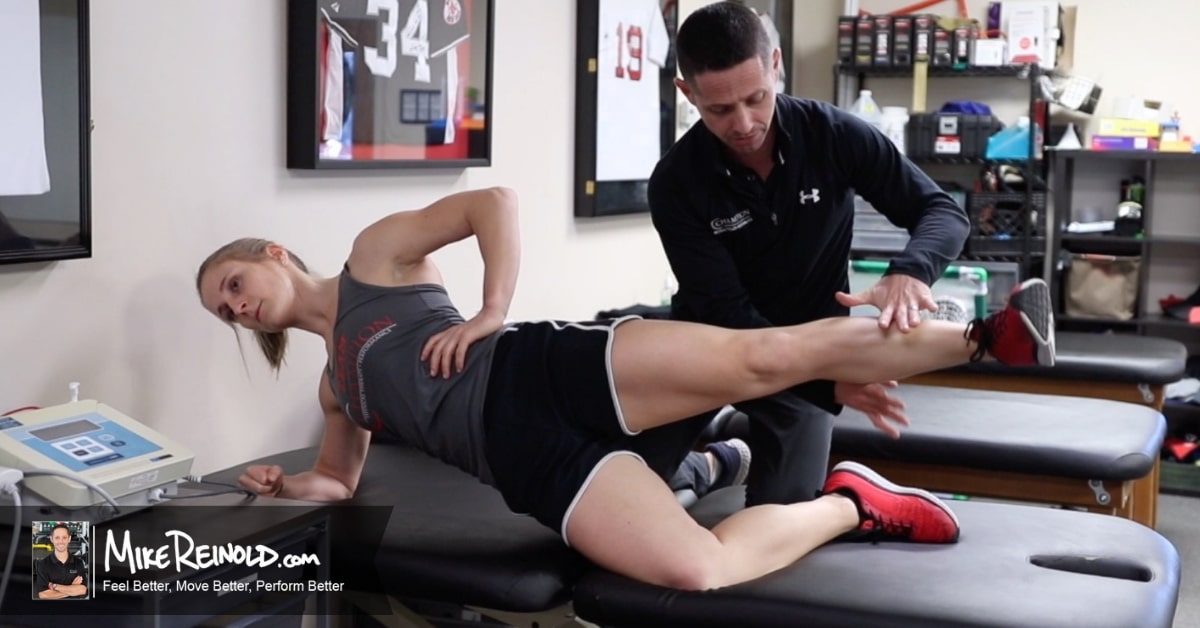
Today’s article is a guest post by Eric Cressey on not only understanding fatigue, but how to manage fatigue as well. This is a really interesting topic to me, as “recovery” is probably the next big area we need to really research and optimize so we can enhance performance for everyone from rehab patients, to fitness enthusiasts, to professional athletes. This is an invaluable lesson that rehabilitation specialists can pick up on from the strength and conditioning world, manage fatigue properly and you’ll see faster outcomes.
Understanding and Managing Fatigue
Perhaps it’s coincidence, or perhaps the scientific community is finally catching on, but recently, there have been several studies looking at the role of short- and long-term recovery in preventing and rehabilitating injuries.
Here’s a research study that demonstrates relationships among a variety of scheduling and recovery factors and injury rates. The part I found most interesting was that researchers observed that sleeping fewer than six hours the night prior to a competition led to a significant increase in fatigue related injuries.
Additionally, researchers at Stanford recently demonstrated the profoundly positive effect that “sleep extension” has on a variety of performance variables in high-level basketball athletes.
These results, in themselves, aren’t particularly surprising: fatigue impacts performance – whether that’s on the field, or in the rehabilitation realm. Anyone who has ever trained an athlete on a Saturday morning after he’s had a late Friday night, or rehabbed a roofer after he’s completed a 10-hour-workday, will tell you that there are certainly less-than-optimal times to get the work in.
What research like this doesn’t tell us, though, is that not all fatigue is created equal – and I suspect that this is one area where strength and conditioning specialists can “return the favor” to rehabilitation specialists for all that we’ve learned from them over the years. Very simply, the very best strength and conditioning coaches I know are the ones who are masters of managing competing demands, including strength training, mobility drills, soft tissue work, movement training, metabolic conditioning, and sport-specific training. In order to effectively manage all these factors, it’s imperative to understand the different stages of fatigue. On the rehabilitation side of things, every injured athlete likely has some element of fatigue that not only impacted his/her injury mechanism, but will impact the response to a given rehabilitation program.
Over-what? Over-everything!
In their classic review, The Unknown Mechanism of the Overtraining Syndrome, Armstrong and VanHeest discussed the importance of differentiating among overload, over-reaching, overtraining, and the overtraining syndrome (OTS). They defined the terms as follows:
- Overload – “a planned, systematic, progressive increase in training stimuli that is required for improvements in strength, power, and endurance”
- Over-reaching – “training that involves a brief period of overload, with inadequate recovery, that exceeds the athlete’s adaptive capacity. This process involves a temporary performance decrement lasting from several days to several weeks.”
- Overtraining – training that “exceeds over-reaching and results in frank physiological maladaptation(s) and chronically reduced exercise performance. It proceeds from imbalances between training and recovery, exercise and exercise capacity, stress and stress tolerance; training exceeds recovery, exercise exceeds one’s capacity, and stressors exceed one’s stress tolerance.”
- Overtraining Syndrome (OTS) – “a set of persistent physical and psychological symptoms that occur subsequent to prolonged application of heavy training loads. The critical diagnostic factor is a chronic decrease in performance, not simply the existence of SAS [signs and symptoms].”
Overload is inherent to a successful training process, and over-reaching is actually quite valuable when used appropriately. For instance, in our training programs at Cressey Performance, we generally fluctuate training stress in four-week programs as high (1), medium (2), very high (3), low (4), where the deloading in week 4 allows for adaptation from the fatigue imposed during week 3.
However, over-reaching is far from overtraining – a term that is thrown around far too often among even the most qualified individuals in the world of health and human performance. Over-reaching may be attained in as little as 7-10 days, and remedied in a matter of days or weeks with adequate deloading. Conversely, the process of overtraining must take place for months for the outcome, OTS, to be apparent. Recovery from OTS requires at least several weeks – and more often several months; in other words, you really have to go out of your way to get to overtraining syndrome.
Since high level performance – and even just normal physical health – is a priority, it is imperative that coaches, parents, and athletes recognize the signs and symptoms of over-reaching and overtraining syndrome – and the differences between the two. According to Armstrong and VanHeest, the signs and symptoms of OTS may include:
- Decreased physical performance
- General fatigue, malaise, loss of vigor
- Insomnia
- Change in appetite
- Irritability, restlessness, excitability, anxiety
- Loss of body weight
- Loss of motivation
- Lack of mental concentration
- Feelings of depression
What All These “Overs” Mean to You
Many of these signs and symptoms are shared between over-reaching and OTS, so how do we know the difference? How do we know when to hold back for a day or two (for overload recovery), 7-21 days (over-reaching), or even months (overtraining syndrome)?
Unfortunately, as much as I would like to be able to offer you the magic answer, I can’t do so. The scientific community has yet to agree on a single, highly sensitive diagnostic test to differentiate among the three. In fact, the only diagnostic tests that are universally accurate are those of physical performance; if performance drops off, there must be some degree of accumulated fatigue.
Other measures – such as heart rate, bloodwork, metabolic rate, substrate metabolism, and a host more – are subject to so many factors that they are hardly reliable tests of one’s training status.
As an example, research from Fry et al. had subjects perform ten sets of one repetition on machine squats at 100% of their one-rep maximum for 14 days straight. That’s an absurd volume of high-intensity resistance training, especially in a trained population. You know what, though? The only thing that dropped off was performance; hormone status (as measured by bloodwork) really didn’t change much at all.
Conversely, crush an endurance athlete with volume, and this same bloodwork will look terrible. The take-home point is that it’s a lot harder to “overtrain” on intensity than volume. And that’s where the problem exists when you’re dealing with athletes: just about every sport out there is a blend of volume and intensity. We don’t just train or rehabilitate shotputters or Ironman competitors; we get athletes from soccer, basketball, baseball, hockey, tennis, and a host of other sports.
So, what is a coach or rehabilitation specialist to do when trying to determine just how much fatigue is present, and what the best course of action is to guarantee an optimal return-to-play as quickly as possible?
In two words: ask questions.
In my opinion, the absolute most important step is to establish communication with athletes and – in this case – patients. Ask about training practices before an injury, sleep patterns, dietary factors, family life, concurrent illness/injury, changes in body weight, and appetite.
These may seem like obvious questions to ask, but we live in a one-size-fits-all world of pre-made templates and rigid systems – and people can fall through the cracks all the time. My experience has been that those most commonly “thrown under the bus” in this regard are the most dedicated athletes forced to train or rehabilitate in a “general health” world. As an example, we had an adult athlete client request a Vitamin D test from a primary care physician last year, and he was turned down because he wasn’t “a post-menopausal female.” As it turned out, he was severely clinically deficient, and normalizing his Vitamin D was a big game-changer for him.
Simply asking the right questions will always help the cause when it comes to determining just how “systemic” what you’re dealing with really is. And, in the process, it gives you an opportunity to show a client or patient how much you care before they even care how much you know.