Rotator cuff tears are very common injuries for people of all ages, even though our ability to evaluate and treat shoulder impingement has improved.. Depending on the study you read, it has been reported that 13% of people over the age of 50 years and 50% of people over the age of 80 years will have a rotator cuff tear. Naturally, rotator cuff repair surgery has become equally as common. Over the last several decades we have made great progress in our rotator cuff repair surgical techniques, transitioning from an open procedure, to a less invasive “mini-open” procedure, and now full arthroscopic.
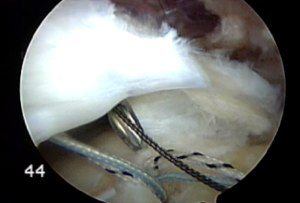 The newer arthroscopic rotator cuff repairs tend to less painful and allow people to do more sooner. However, one mild little fact that we often do not hear about is that the failure rate after rotator cuff repair surgery is still too high.
The newer arthroscopic rotator cuff repairs tend to less painful and allow people to do more sooner. However, one mild little fact that we often do not hear about is that the failure rate after rotator cuff repair surgery is still too high.
Past studies have shown up to 75% of people following a rotator cuff repair will technically “fail” if you define surgical failure as the cuff is not intact again after surgery. A recent systematic review published in JOSPT reported a failure rate between 18% and 40% over 10 different research reports.
Despite these “failure” rates, most research studies have shown that patient satisfaction after surgery is still very high. This tells me that the rehabilitation process may be far more important than the actual surgery. That is great news, even if the rotator cuff is found to not be intact again after surgery, pain, motion, strength, function, and satisfaction can all still be improved significantly.
Regardless, we should all be doing everything we can to maximize your success after rotator cuff repair surgery.
A recent systematic literature review publish in JOSPT sought to determine the prognostic factors associated with a successful recover following arthroscopic rotator cuff repair surgery. Based on this paper, we can identify several factors that can help maximize your outcomes following surgery. While, not all of these factors are easily addressed, many are, and it is always my goal to assure you put yourself in the best position to succeed.
Factors Associated with Successful Recovery Following Rotator Cuff Repair
The review focused on 10 papers that met the authors’ strict guidelines for inclusion. Based on these 10 papers, they were able to identify 12 factors that were correlated to better outcomes following rotator cuff repair surgery. These 12 factors were divided into 4 categories: demographic factors, clinical factors, factors related to the rotator cuff integrity, and factors related to the surgical procedure.
I am going to discuss the first 3 as they relate to things we may be able (or not able) to do to enhance outcomes following rotator cuff surgery. In regard to surgical factors, one study showed that performing additional procedures to the biceps or acromioclavicular joint was associated with poorer outcomes. We can’t really control the surgical procedures, but perhaps this information may be beneficial to the surgeons.
Demographic Factors
The most significant finding in regard to general demographics was related to patient age at the time of surgery. Older age had a negative effect on recovery.
The studies demonstrated that the older you are, the less your chance of tendon healing. Those under the age of 55 years have the best outcomes with between 88-95% chance of tendon healing. In contrast, people aged over 60 years had between 43-65% chance of tendon healing.
While you can’t control when your rotator cuff becomes troublesome, these results do imply that we should not ignore symptoms and allow your shoulder and rotator cuff to gradually become more degenerative. Addressing issues earlier should help with outcomes. We have all seen it, most people put off addressing their shoulder soreness for years, attempting to work through the discomfort. We don’t usually seek help until our functional level is significantly impaired.
Clinical Factors
Not surprising, bone mineral density and diabetes were both associated with poorer tissue healing. Obesity was also associated with less successful outcomes. People that were considered obese had a 12% less chance of successful outcomes.
I thought a very interesting finding involved your activity level prior to surgery. People who rarely participated in physical activities had poorer outcomes that those that participated in medium- and high-intensity sports, such as golf, swimming, cycling, running, and tennis.
In regard to strength and motion, it was determined that the best predictor of final strength was initial strength. Preoperative should stiffness also had a negative effect on recovery time, delaying return to activity.
While some of these factors, like bone mineral density and diabetes, may not be avoided, you can assure that these are under control medically before surgery. However, factors such as obesity, activity level, strength, and mobility are all likely related and can be addressed prior to surgery. This underscores the importance of performing physical therapy PRIOR to surgery. I always say, the better you look going into the surgery, the better you’ll look coming out of surgery.
Rotator Cuff Integrity Factors
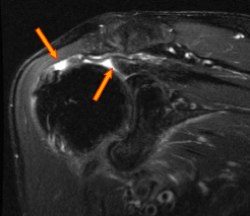
Essentially, the more degenerative the tissue, the worse the outcomes. Over time, your cuff tear will progress in size, potentially start to pull off the bone (retract), and become weak.
These factors are probably more associated with my comments on age above. Perhaps we should be more proactive with our decisions regarding taking care of our shoulders prior to the tear becoming more involved and the tissue more degenerative. Something to consider, repair of a small rotator cuff tear had a 96.7% chance of healing after surgery in comparison to a 58.8% chance if that tear becomes large.
What You Can Do to Enhance Outcome Following Rotator Cuff Repair Surgery
I feel like this study shed some light on several things we can do to enhance your outcomes following rotator cuff repair surgery:
- First we should do our best at evaluating shoulder impingement, and then treating shoulder impingement symptoms to try to minimize a rotator cuff tear in the future.
- Do not unnecessarily put off surgery as outcomes are less successful the older you are at the time of surgery.
- In regard to the above, also consider that putting off surgery may allow the rotator cuff to become degenerative. The larger the tear and the more degenerative the tissue, the less successful the outcome.
- Being physically active and losing weight are both associated with better outcomes. Get off your butt.
- Begin physical therapy prior to surgery. The stronger and more mobile your shoulder is at the time of surgery, the better off you’ll be after surgery. You’ll be stronger and return to activities sooner. Plus, some studies have shown that physical therapy can help you avoid rotator cuff surgery.
- Assure that medical conditions, such as bone mineral density and diabetes, are being addressed and under control prior to surgery.
For the clinicians reading this, we can also use this information to determine our rate of progression during rotator cuff repair rehabilitation. The more prognostic factors that your patient may have indicating a less successful outcome, the more conservative you may need to progress.
Would you progress some that is a 52 years old physical active person with a small rotator cuff tear and no other health issues at the same pace as a 74 year old with a large tear, weakness, and diabetes? Of course not. We can’t just blindly follow a protocol. Protocols are useful and necessary, but they just provide structure that you adjust if factors dictate that you should be more conservative.
There are ways to enhance your success after rotator cuff repair surgery, many of which are controllable. Use these findings to help you or your client’s maximize your outcomes following surgery.